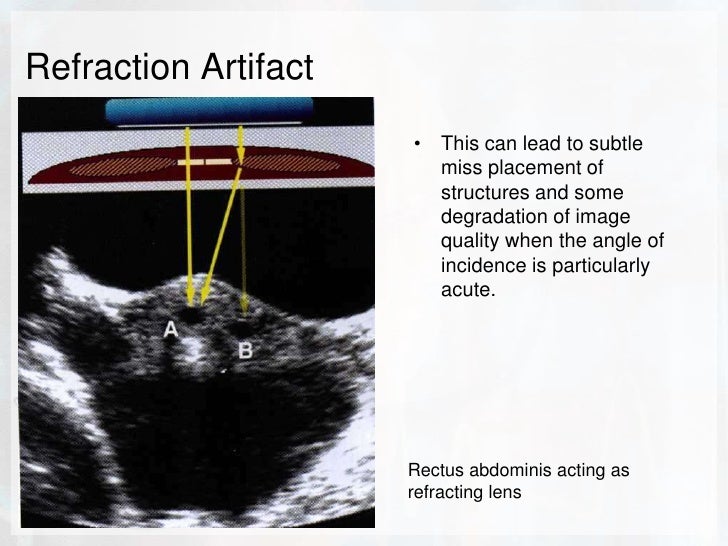
To be able to use the BLUE protocol for building profiles of pneumonia (or acute respiratory distress syndrome) and understand their limitations. To understand the sequential thinking when making ultrasound diagnosis of pneumothorax. To be able to cite, in the correct hierarchy, the seven criteria of the B-line, then those of interstitial syndrome. To understand the logic of the BLUE points, three points of interest enabling expedition of a lung ultrasound examination in acute respiratory failure. To be able to use a terminology that has been fully standardised to avoid any confusion of useless wording. 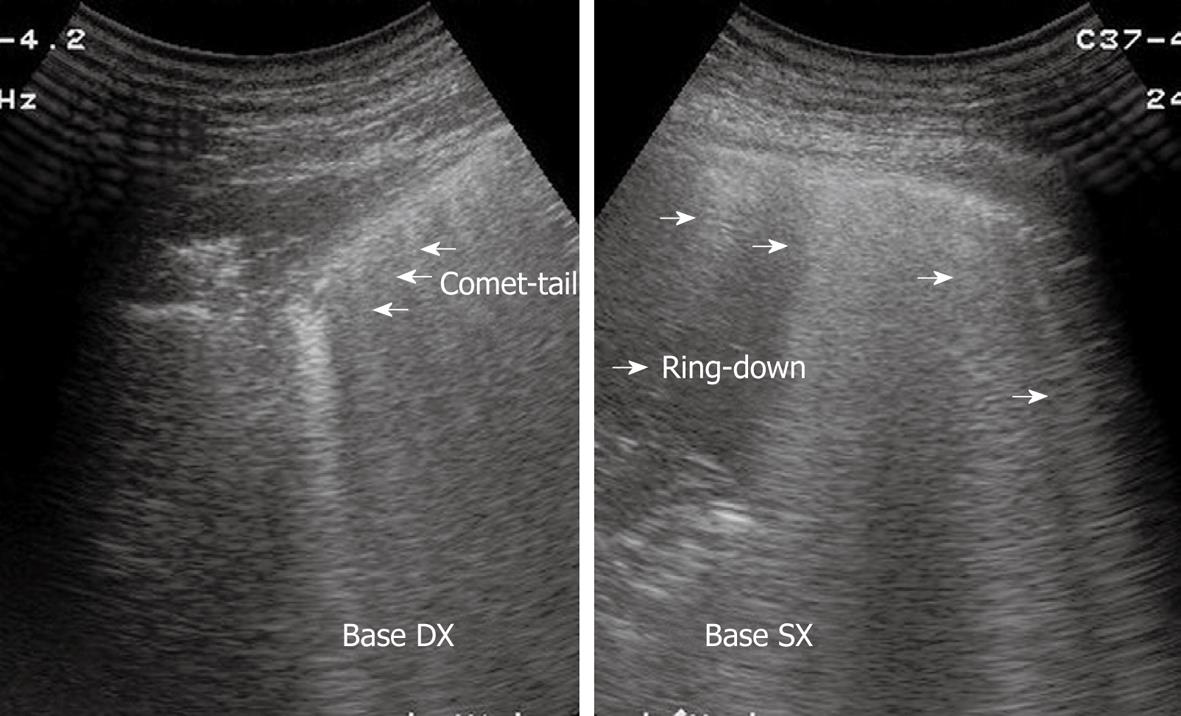 
The M-mode setting further enhances visualization and aids in the diagnosis of pneumothorax.To understand that the use of lung ultrasound, although long standardised, still needs educational efforts for its best use, a suitable machine, a suitable universal probe and an appropriate culture. Once visualization of the pleura is established, the lung may be assessed for the presence or absence of normal lung sliding and comet-tail artifacts. Patients presenting with suspected pneumothorax can be assessed quickly through bedside ultrasound. Pneumothorax is a medical emergency requiring immediate diagnosis and treatment. Remember, visualization of the lung point is pathnognomic for pneumothorax. The ribs should always be identified to ensure one is looking at the pleural line.Īlthough absence of lung sliding can suggest pneumothorax, other conditions, such as severe consolidation, acute respiratory distress syndrome, and mainstem intubation, can give a similar appearance. In some cases of pneumothorax, subcutaneous air may obscure the pleura. Using the M-mode in these cases may help to identify inflated lung in patients with limited movement at the pleural line.įurthermore, since it is easy to confuse a bright layer of fascia with the pleura, the clinician should always make sure to identify landmarks. The clinician should also be mindful of the presence of bullae as the appearance of sliding may be diminished in patients with bullous disease. If one evaluates only the anterior chest, air trapped in another location may be missed. The presence of scarring and adhesions may cause the patient to develop loculated air collections. There are several pitfalls that can limit the ability to correctly diagnose a pneumothorax. This pattern is described as the “barcode sign” or “stratosphere sign” (Figure 4). Instead, the M-mode shows a linear pattern below the pleural line. In pneumothorax, however, the granular sand appearance is absent. While performing the ultrasound, it is important to always keep the probe as still as possible to identify independent motion at the pleura. 
(The manner in which the image is produced may be thought of as a graph, with the x-axis representing time and the y-axis the depth.) When using M-mode, the screen will vary in appearance depending on the type of ultrasound being used. The M-mode takes a single line of echoes from the two-dimensional image and plots it against time. Since lung sliding is sometimes challenging to visualize, using the motion mode (M-mode) on ultrasound can help to confirm findings. This point moves with respiration, and if visualized, confirms pneumothorax. Comet tails, vertical artifacts originating from the pleura, may be visible on ultrasound, also proving the lung is inflated (Figure 2).īy continuing to scan laterally down the chest, the clinician may encounter the “lung point”-the junction between the normally inflated lung and pneumothorax. The pleura will seem to slide back and forth as the patient breathes. Lung sliding has been described as a shimmering appearance of the pleura, or like tiny ants marching on a string. The appearance of lung sliding or a comet-tail artifact on the ultrasound confirms the lung is inflated.
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
